Living with food allergies extends far beyond simply avoiding certain foods. For many patients and their families, the psychological impact of managing IgE-mediated food allergies can be just as challenging as the physical aspects. If you or your child has been diagnosed with food allergies, you may be experiencing anxiety, stress, or feeling overwhelmed by the constant vigilance required. The good news is that mental health support specifically tailored to food allergy management is available and can make a significant difference in your quality of life.
Why Mental Health Matters in Food Allergy Management
Research shows that patients with food allergies and their caregivers consistently identify mental health support as a clinical priority. The American Academy of Allergy, Asthma & Immunology recognizes this need and has developed guidelines for integrating mental health professionals into food allergy practices.
The connection between food allergies and mental health is well-documented. Parents of children with food allergies often experience significant burden and anxiety related to keeping their child safe. Children and adolescents with food allergies may struggle with feelings of being different from their peers, social isolation, or fear of allergic reactions. These psychological challenges can impact daily functioning, quality of life, and even treatment adherence.
Who Benefits from Food Allergy Mental Health Support?
Understanding when mental health support can be helpful requires recognizing that not everyone with food allergies needs traditional therapy. The Pediatric Psychosocial Preventative Health Model provides a useful framework for thinking about mental health needs in chronic illness management.
Universal Support for All Families
Ideally, all patients and caregivers would meet with a food allergy-informed mental health professional soon after diagnosis. This initial consultation serves several important purposes:
- Providing developmentally appropriate psychoeducation about living with food allergies
- Teaching fundamental coping skills for managing the diagnosis
- Learning to balance necessary vigilance without excessive avoidance
- Determining if follow-up care is needed
This type of support is particularly valuable because food allergy management challenges evolve throughout different developmental stages. Research indicates that food allergy-related quality of life may actually worsen as pediatric patients get older, highlighting the importance of ongoing support throughout childhood and adolescence.
Targeted Support for Specific Challenges
Some situations call for more focused mental health intervention. You might benefit from short-term therapy if you are:
- Struggling to cope with a new food allergy diagnosis
- Experiencing anxiety that affects your daily functioning or willingness to engage in life experiences
- Having difficulty communicating about food allergy needs with schools, daycares, or other caregivers
- Preparing for an oral food challenge or starting immunotherapy treatment
- Dealing with food allergy-related bullying
- Experiencing post-traumatic symptoms after an allergic reaction or anaphylaxis
- Developing restrictive or selective eating patterns related to food allergy fears
- Navigating the transition of food allergy management responsibility from parent to child
Long-Term Support for Complex Needs
A smaller subset of patients may need ongoing, long-term therapy. This typically includes situations where food allergy concerns are part of a broader mental health disorder or when distress is persistent and significantly impacts daily life.
Evidence-Based Treatment Approaches for Food Allergies
Mental health professionals who work with food allergy patients use several proven treatment approaches:
Cognitive-Behavioral Therapy
Cognitive-behavioral therapy, or CBT, is one of the most well-established treatments for food allergy-related anxiety and distress. CBT helps you understand the connections between your thoughts, feelings, and behaviors while developing more helpful thinking patterns.
For anxiety about food allergies, CBT might involve:
- Identifying and challenging anxious thoughts about allergic reactions
- Learning relaxation techniques like deep breathing and visualization
- Gradually approaching situations you have been avoiding due to food allergy fears
- Building confidence in your ability to manage food allergies effectively
A specialized form of CBT called allergen proximity challenges has shown particular promise. This approach involves gradual exposure to being physically near allergens in controlled settings, which can significantly reduce anxiety and improve quality of life without requiring you to actually consume the allergen.
Acceptance and Commitment Therapy
Acceptance and commitment therapy, known as ACT, takes a different approach by helping you develop psychological flexibility. Rather than fighting against the reality of food allergies, ACT helps you accept the diagnosis while still living a meaningful, value-driven life.
For caregivers, ACT can be particularly beneficial in accepting circumstances you cannot change while focusing on what truly matters to your family. This approach reduces the tendency to let fear dictate life decisions and choices.
Motivational Interviewing
Motivational interviewing is especially useful when addressing treatment adherence or motivation to pursue testing and treatment. This approach explores your own motivations and helps resolve ambivalence about recommended allergy care, whether that involves following management strategies, attending appointments, or participating in immunotherapy protocols.
Family-Based Interventions
Food allergy management affects the entire family system. Family-based interventions can address:
- Division of food allergy management responsibilities
- Supporting age-appropriate independence in self-management
- Managing caregiver anxiety that may lead to overprotection
- Navigating solid food introductions with infants who have food allergies
- Communication strategies between family members about food allergy needs
Support for Feeding Difficulties
Some individuals with food allergies develop eating difficulties ranging from selective eating to avoidant/restrictive food intake disorder, or ARFID. When feeding problems become severe, multidisciplinary intervention using CBT or behavioral therapy approaches represents the gold standard of care. Mental health professionals work alongside dietitians and physicians to safely expand dietary variety and address the psychological factors contributing to restricted eating.
How to Access Mental Health Support for Food Allergies
Finding the right mental health support for food allergy concerns depends on several factors, including your location, insurance coverage, and the specific services you need.
Models of Care
Mental health support for food allergies can be delivered through several different models:
- Consultation-Liaison Services: Some allergy clinics have mental health professionals available during regular appointments, particularly for oral food challenges. These brief consultations can provide immediate support, screening for mental health needs, and referrals for ongoing care when needed.
- Multidisciplinary Team Visits: In this model, you meet with multiple providers including an allergist, mental health professional, and possibly a dietitian during a single appointment. This approach allows for coordinated care and reduces the need for multiple separate visits.
- Outpatient Therapy Referrals: Your allergist may refer you to a mental health professional for ongoing therapy, either within the same medical institution or in the community. These sessions occur independently of allergy visits and can be short-term or long-term based on your needs.
Finding a Qualified Provider
When seeking mental health support for food allergies, ideally you want to work with a professional who has specific training and experience in this area. The Food Allergy Counseling Directory at www.foodallergycounseling.org/directory is a valuable resource for locating food allergy-informed therapists.
Licensed mental health professionals who provide therapy include:
- Clinical psychologists with PhD, PsyD, or EdD degrees
- Licensed clinical professional counselors
- Licensed clinical social workers
- Licensed marriage and family therapists
If you cannot find a food allergy-specific therapist in your area, look for mental health professionals who specialize in health anxiety, chronic illness, or pediatric psychology. These professionals can still provide valuable support even without specific food allergy training.
Insurance and Billing Considerations
Mental health services for food allergies are typically billable to insurance, though coverage varies by plan. Services may be billed using mental health diagnostic codes or Health and Behavior codes, which allow billing under physical health diagnoses like food allergy. Check with your insurance provider about your specific coverage for mental health services, including copayments and deductibles.
Some allergy clinics, particularly those in academic medical centers, may offer mental health support through alternative funding sources such as grants or philanthropy, which can increase accessibility.
Telehealth Options
Telehealth has expanded access to food allergy mental health support, particularly for families living far from specialized medical centers. However, licensing requirements mean that mental health professionals can only provide services to patients physically located in states where they hold a license.
Recent developments in interstate compacts are improving access. The American Psychological Association’s PsyPact allows qualified psychologists to practice in 42 states as of January 2025. The American Counseling Association’s Interstate Counseling Compact began granting privileges to counselors in 37 states in 2025. These compacts make it easier to access specialized food allergy mental health support regardless of your location.
Self-Help Resources and Tools
While working with a mental health professional provides the most comprehensive support, several resources can help you begin addressing food allergy-related stress and anxiety:
Educational Resources
- Age-appropriate children’s books about food allergies that address emotional aspects
- Online resources from organizations like Food Allergy Research & Education and the Center for Food Allergy and Asthma Research
- Educational handouts from the American Academy of Allergy, Asthma & Immunology on food allergy stages and psychosocial adjustment
Assessment Tools
Your allergy provider may use standardized questionnaires to screen for mental health concerns related to food allergies. These tools assess areas like quality of life, anxiety levels, and caregiver burden. While these assessments are not diagnostic, they can help identify when additional support might be beneficial and track improvement over time.
Mobile Apps and Online Tools
Several apps can support food allergy management and reduce stress by simplifying daily tasks like finding safe restaurants, translating allergy information for travel, and discovering allergy-friendly recipes.
What to Expect from Food Allergy Mental Health Treatment
Mental health treatment for food allergies typically focuses on developing what experts call a “relaxed readiness” approach. This means maintaining appropriate vigilance and preparedness to act when needed while also managing anxiety effectively so you can enjoy a good quality of life.
Treatment goals are individualized but commonly include:
- Reducing excessive worry while maintaining necessary caution
- Improving confidence in food allergy management abilities
- Decreasing avoidance of safe activities and social situations
- Developing effective communication strategies about food allergy needs
- Supporting age-appropriate independence in self-management
- Processing trauma from past allergic reactions
- Addressing feeding difficulties or food avoidance
The length and intensity of treatment varies based on your specific needs, ranging from a few sessions focused on a particular challenge like preparing for an oral food challenge to longer-term therapy for more complex concerns.
Bottom Line
Living with food allergies presents real psychological challenges that deserve professional support. Mental health care is not a sign of weakness or inability to cope but rather a valuable tool for managing a complex medical condition. The integration of mental health professionals into food allergy care represents an important step toward addressing the full spectrum of patient and family needs.
If you are struggling with anxiety, stress, or other mental health concerns related to food allergies, talk to your allergist about available resources. Whether you need brief psychoeducation, targeted support for a specific challenge, or ongoing therapy, help is available. With appropriate mental health support, you can develop effective coping strategies, reduce distress, and improve your quality of life while safely managing food allergies.
Remember that experiencing stress and anxiety about food allergies is normal and common. You are not alone in these challenges, and seeking support is a positive step toward thriving despite the complexities of living with food allergies.
References
This article is based on guidance from the American Academy of Allergy, Asthma & Immunology Work Group Report on Integration of Mental Health Care into Food Allergy Practices, published in the Journal of Allergy and Clinical Immunology: In Practice (2025). Additional research supporting mental health interventions for food allergies has been published in peer-reviewed journals including Pediatric Allergy and Immunology, Annals of Allergy, Asthma & Immunology, and Clinical and Experimental Allergy.
For professional guidance specific to your situation, consult with your allergist and a qualified mental health professional experienced in food allergy care.
 Spring brings warmer weather, blooming flowers, and longer days. But for millions of people, it also signals the start of seasonal allergy symptoms. If you find yourself sneezing, congested, or dealing with itchy eyes, you are not alone. According to the Centers for Disease Control and Prevention, allergies affect roughly one in three adults in the United States, making them one of the most common chronic conditions.
Spring brings warmer weather, blooming flowers, and longer days. But for millions of people, it also signals the start of seasonal allergy symptoms. If you find yourself sneezing, congested, or dealing with itchy eyes, you are not alone. According to the Centers for Disease Control and Prevention, allergies affect roughly one in three adults in the United States, making them one of the most common chronic conditions.


 If your baby seems fine during feeding but begins repeated vomiting one to four hours later, you may be asking an important question: Could this be a food allergy?
If your baby seems fine during feeding but begins repeated vomiting one to four hours later, you may be asking an important question: Could this be a food allergy?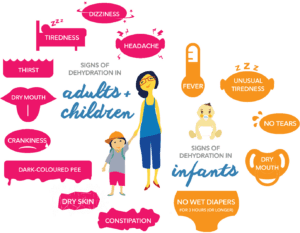


 Longer days and warmer temperatures are welcome signs of spring. But for many people, spring also brings sneezing, congestion, and itchy eyes. If you’ve ever wondered, “How can I prevent spring allergy symptoms before they start?” you’re not alone. Tree pollen season begins earlier than many expect, and preparation is key to staying ahead of symptoms.
Longer days and warmer temperatures are welcome signs of spring. But for many people, spring also brings sneezing, congestion, and itchy eyes. If you’ve ever wondered, “How can I prevent spring allergy symptoms before they start?” you’re not alone. Tree pollen season begins earlier than many expect, and preparation is key to staying ahead of symptoms.
 If your child is receiving Palforzia for peanut allergy, you may be asking: What happens when Palforzia is discontinued? What are our options? Is oral immunotherapy still possible?
If your child is receiving Palforzia for peanut allergy, you may be asking: What happens when Palforzia is discontinued? What are our options? Is oral immunotherapy still possible?


 Claire is an American Academy of Nurse Practitioners board certified Family Nurse Practitioner with a special interest in allergy and immunology. She is a summa cum laude graduate of Providence College where she received her Bachelor of Science in Biology. She then went on to receive her BSN and MSN from MGH Institute of Health Professions and has been working as a Nurse Practitioner in Allergy ever since.
Claire is an American Academy of Nurse Practitioners board certified Family Nurse Practitioner with a special interest in allergy and immunology. She is a summa cum laude graduate of Providence College where she received her Bachelor of Science in Biology. She then went on to receive her BSN and MSN from MGH Institute of Health Professions and has been working as a Nurse Practitioner in Allergy ever since.
